Introduction
SLT is a simple, quick and effective outpatient treatment for reducing the pressure in the eye of patients with glaucoma or ocular hypertension. SLT is completely different from the laser used for short sight correction and is not associated in any way with the risks associated with “vision correction”. SLT is the latest version of laser trabeculoplasty, a procedure which has been used to treat patients with glaucoma since 1979 (1). SLT was first reported in 1998 (2) and has been in widespread use since 2004.
How and where is SLT done?
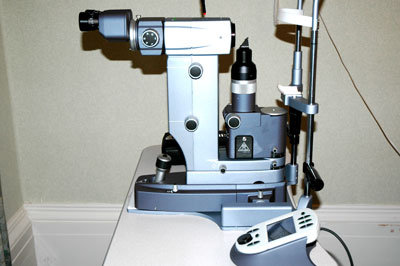
SLT is done as outpatient at the Somerfield Hospital. The laser is applied at a slit lamp very similar in appearance to that used by ophthalmologists and opticians to examine your eyes routinely. A nurse puts some drops into your eye to anaesthetise it and make the pupil smaller. Then a contact lens is applied to the eye to help focus the beam and to prevent you from blinking. The whole process takes about 10 minutes. You will not feel any pain during the procedure but some patients get mild glare and discomfort for a few days afterwards. The pressure in the eye should respond within two to three days and will be checked at an out-patient visit after 2 to 3 weeks.
How successful is SLT?
An increasing number of ophthalmologists in the UK are able to offer SLT, but the technique has been most widely employed in the USA. Numerous studies have demonstrated it’s safety and efficacy (3). Most report an average drop of eye pressure (intraocular pressure or IOP) of between 7 and 8 mmHg. About 80% of patients get a 20% or more reduction in IOP. Some eyes respond more than others, but only about 4% fail to respond at all. If the pressure fails to fall by 3 mmHg or more after 2 to 3 weeks, I generally redo the laser procedure. About 10% of patients require 2 or more sessions to bring down the IOP to an acceptable level. Some patients may require drops in addition to SLT to bring the IOP down sufficiently, although SLT generally reduces the number of drops required.
What are the side effects?
Apart from slight discomfort after treatment, few side effects are encountered and the procedure can easily be repeated if not initially successful. To quote one study (4): “…ocular discomfort is not unusual in the first few days after SLT. Late complications causing ocular morbidity after SLT were not encountered.” Transient ocular pain occurs in about 40% eyes. There have been 4 reported cases of hyphaema (out of millions of treatments). Patients with heavily pigmented drainage angles should be treated with caution (reduced energy and number of pulses) to prevent intraocular pressure spikes.
Compliance
Patients do not receive any short-term gain from taking glaucoma medications; they do not see or feel better and medications can produce unwanted side effects. This means that it is easy to forget to take drops. With SLT, patients don’t have to remember their drops. This probably explains why the visual fields of patients treated with laser trabeculoplasty were better preserved than those of patients treated with drops in the Glaucoma Laser Trial (6). Although my patients always insist they take their drops, studies have shown that non-compliant patients miss about 100 days of treatment per year and about a quarter of all glaucoma prescriptions are never picked up from the pharmacy. In a recent editorial in Ophthalmology (7), the editor stated that the 2 most important ways or reducing the toll of blindness from glaucoma in the community were to i) ensure screening of all first degree relatives of patients with glaucoma and ii) encourage more patients to have laser trabeculoplasty, which would improve compliance with treatment.