Definition
Inflammation of the conjunctiva. This causes the eye to become sore (gritty) and red with a variable discharge.
Types of conjunctivitis and their treatment
Infection
Bacterial
This is the commonest type of conjunctivitis and is typically seen and treated by GP’s before the patient sees an ophthalmologist. It presents with sore, red, gritty eyes (usually both are affected) and their may be a yellow-green discharge present. In children, infection with Haemophilus influenzae is relative common and this usually responds well to treatment with chloramphenicol drops. Otherwise, infection is most commonly caused by Staphylococcus aureus. In older age groups, infection of the conjunctiva and lid margin can be caused by Pseudomonas sp. which require treatment with ofloxacin drops and polyfax ointment. See also.
Viral
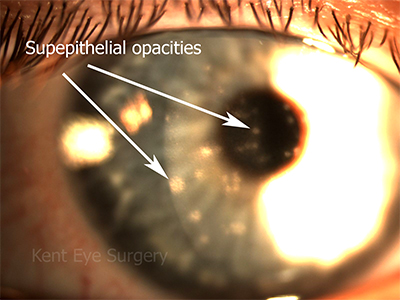
A first infection with herpes simplex may cause a follicular conjunctivitis that will subside with a 2 week course of acyclovir ointment. Far more commonly, however, viral conjunctivitis is associated with infection with adenoviruses. These typically start in one eye, before affecting the other, and can be extremely contagious. Patients frequently have a tender lump in front of the ear in the first side affected (an enlarged preauricular lymph node), which is an excellent warning sign to the examining clinician that he or she should be scrupulous in their hand hygiene. Unfortunately, no specific treatment exists and patients are often confined to a dark room for a week or more before eventual recovery. In a proportion of cases, coin-like lesions on the front surface of the cornea appear, which respond partially to steroid drops. These do blur the vision to some extent, which can take a year or two to recover. The scars fade slowly over a few years.
Chlamydial
This typically presents as a red eye in one only. A florid follicular conjunctivitis with discharge is present and once again, the preauricular lymph node is enlarged. It is almost always associated with concomitant genital infection and patients should be examined by a genito-urinary consultant before treatment is started. It resolves on treatment with a tetracycline based antibiotic such as doxycycline given for one week. Click here to see a photograph of a patient with follicular conjunctivitis.
Allergic
Commonly, allergic conjunctivitis is seasonal, although the times patients are affected are not necessarily confined to the typical hayfever season as many people develop symptoms in January and February. Patients present with red, watering eyes which are usually itchy. There may be a white stringy discharge coming from the eye. The condition usually responds to treatment with mast cell stabilisers such as opticron (sodium chromoglycate), but I usually use opatanol because this drop also has a local anti-histamine effect and only needs to be given twice a day. Unfortunately, it is not available over the counter. Some patients need treatment with steroid drops such as FML (Fluoromethalone). Since these can cause the pressure in the eye to rise and are associated with cataracts when given for long periods of time (over 6 months), patients need to be monitored by an ophthalmologist when receiving steroid eye drops.
Drop induced
Patients taking drops for glaucoma may develop a sore, red eye with peeling red peri-orbital skin. In descending order of frequency, this is seen with alphagan (bromonidine), trusopt (dorzolamide), lumigan (bimatoprost), travatan (travaprost) and xalatan (latanaprost). The treatment is simply to stop using the drop and recovery is noted in 3-5 days. Unfortunately, this does complicate the treatment of glaucoma and the patient will need to be reviewed relatively promptly to reasses the treatment plan.