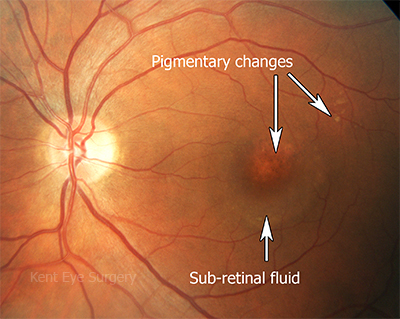
This condition usually occurs in patients between the ages of 30 and 50 and presents with mild blurring of vision in one eye. This is caused by a small collection of fluid beneath the macula (retina) secondary to malfunction of the tissue supporting the retina (the retinal pigment epithelium or RPE). Another common symptom is feeling that objects appear smaller in the affected eye (micropsia).
The underlying cause of the problem is an unexplained defect in the vascular layer supporting the retinal pigment epithelium (the choroicapillaris) which becomes more leaky and creates a small blister in the retinal pigment epithelium. In some patients, this is all that happens (an RPE detachment or PED), but in others, a defect in the RPE lets fluid escape under the retina and this is usually associated with clinical symptoms.
Examination may reveal that both eyes are affected even if symptoms are confined to one eye only. The condition is usually diagnosed by clinical examination alone, although for more difficult cases further investigations using fluorescein angiography and ocular coherence tomography may be employed.
Fluorescein angiography may be used to classify the condition into 3 types:-
i) source or point leakage without RPE atrophy/retinal pigmentation
ii) source or point leakage with RPE atrophy/retinal pigmentation
iii) diffuse leakage (usually associated with chronic symptoms)
Vision usually improved to 95% of its original level by 3 months without specific treatment. Recurrences occur in 30% of patients and in a very small number, the condition may become chronic. In these patients the treatment options include Diamox tablets, betablocker tablets and photodynamic laser therapy. This is a picture of a fundus in a patient with persistent CSR:-
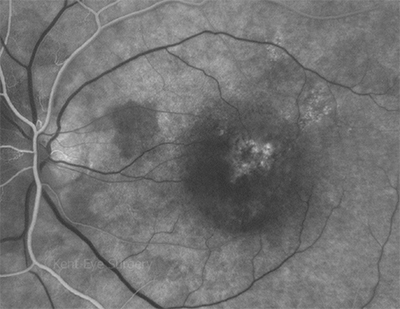
This is an early fluorescein angiogram (FFA) picture of this patient:-
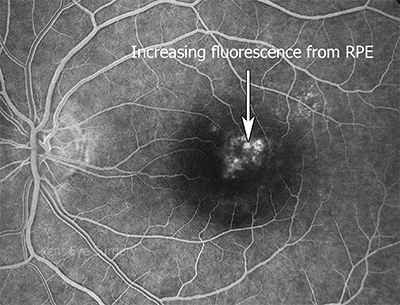
And this is the late FFA picture:-
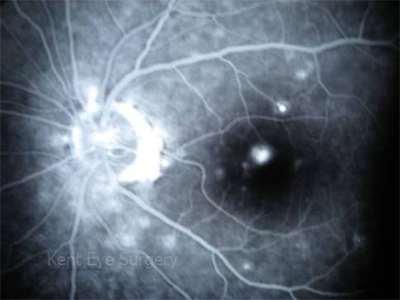
Very rarely, the condition is complicated by a choroidal neovascular membrane, which can respond well to treatment with anti-VEGF injections into the eye. The following is a late phase fluorescein angiogram of a such a patient, who presented with vision of 6/24 and metamorphopsia. His vision improved to 6/6 within 3 weeks of one injection of intravitreal Avastin 1.25mg.